Testicles
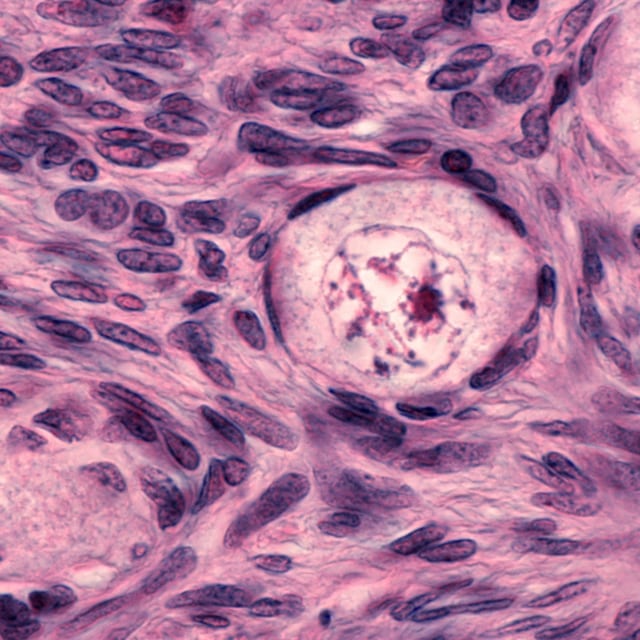
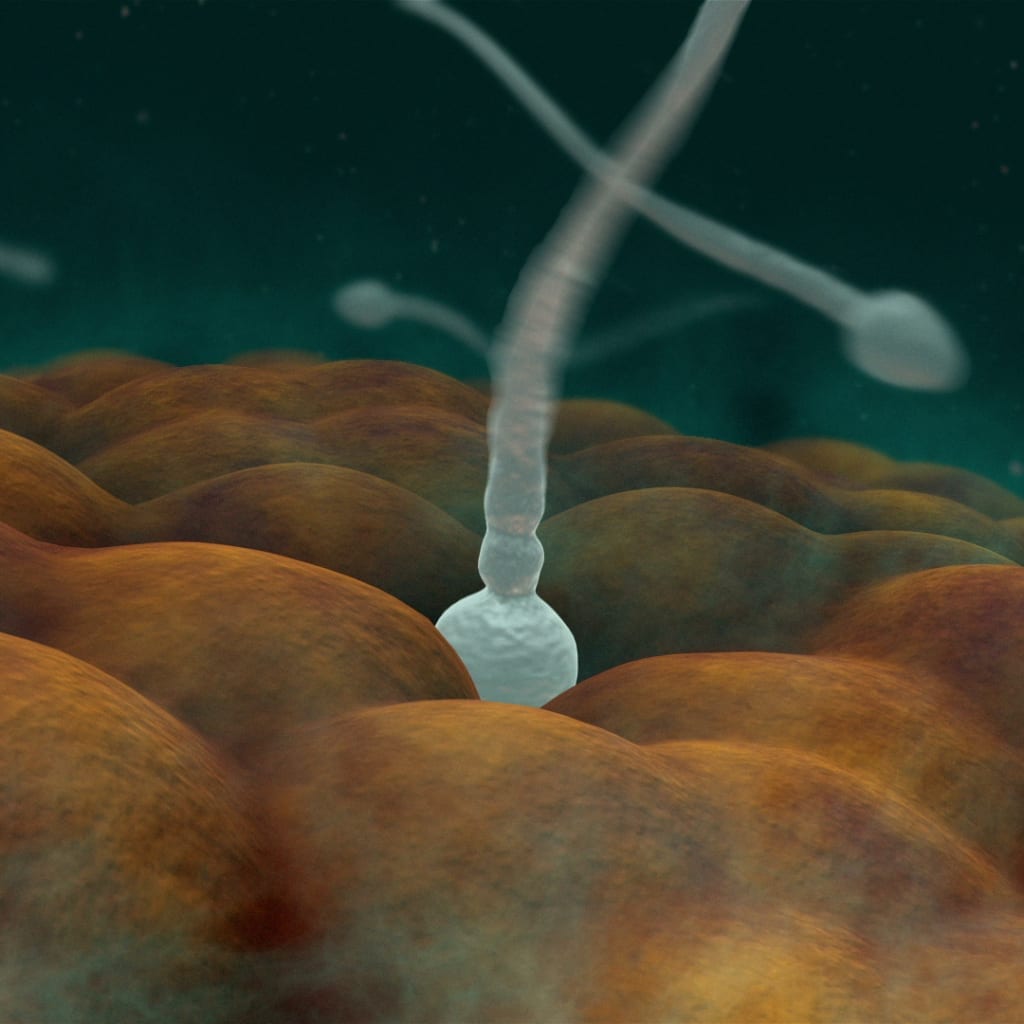
Testicles (aka. testes, sing. testis) are male sexual glands, are usually present as a pair, oval in shape and produce the male sexual hormone testosterone as well as the sperms (aka. sperm cells or spermatozoa). Testicles reside in scrotum, which is a sac of skin that hangs below the penis. For normal sperm development, the temperature of scrotum and testicles is slightly lower than the body temperature.